Surgery for childhood bone cancer
Most children with bone cancer will have surgery. Whether surgery is possible usually depends on where the tumour is.
-
Tumours in an extremity such as an arm, leg, hand or foot are usually easier to completely remove with surgery. Tumours that can be removed with surgery are called resectable.
- Tumours in the spine, pelvis and base of the skull are very hard to completely remove. Tumours that can't be removed with surgery are called unresectable. Doctors will use other treatments, such as radiation therapy and chemotherapy, for these tumours.
The most important goal of surgery is to remove the tumour completely with a margin of normal tissue around it. Where the tumour is determines what tissues or structures need to be removed.
Planning the surgery and reconstruction
The surgeon who planned or carried out the biopsy will also do the surgery to remove the tumour. The area where the biopsy was taken will need to be removed when the tumour is removed.
Before surgery, your child will have tests (MRI, CT or PET-CT) to reassess the tumour. These tests tell doctors where the borders of the tumour are, how it has responded to chemotherapy before surgery and if it has spread. This helps plan surgery and the next steps of treatment. The size of the tumour and where it is are key to planning how to completely remove the bone cancer along with a margin of normal tissue. It may be necessary to remove some of the soft tissues surrounding the bone or a joint next to the affected bone. It may also be necessary to reconstruct the bone or joint.
For smaller bones of the leg, arm, ribs, collarbone, toes or fingers, reconstruction is not usually needed after the cancer has been removed.
For the large bones of the arm and leg, reconstruction is done at the same time as surgery to remove the cancer. The healthcare team may suggest different options, with pros and cons, that you and your child need to choose between.
In thinking about the options, it will be important to consider:
your child's age, lifestyle and activity levels
- how much care and support you have available after surgery
- how your child's body image may be affected
You may find it helpful to talk to someone who has had the surgery and reconstruction that the healthcare team is suggesting and to look at pictures or videos of people who have had the surgery.
Types of surgery
The following types of surgery are used to treat childhood bone cancer:
Wide resection
A wide resection removes the bone tumour along with a wide margin of normal bone and tissue around the tumour. Any tissue from or near the biopsy site is also removed along with the tumour. This type of surgery is also called wide local excision or en bloc resection.
Depending on the amount of tissue removed, your child's surgeon may need to use skin or tissue from another part of the body (called a graft) to replace it. This is done at the same time as the surgery to remove the cancer.
Amputation
An amputation removes part or all of a limb. Surgeons use amputation when the tumour is affecting vital structures and these vital structures must be removed in order to remove the entire tumour. An amputation may also be needed if the bone cancer has come back in the same limb after limb-sparing surgery.
A child can still have very good quality of life and do many of their normal activities after amputation.
Advantages of amputation include:
It has a shorter healing time than other types of surgery. (But a child may still need a lot of rehabilitation to learn to walk again.)
- There are no restrictions to activity. The child can participate in activities involving running and contact sports because there is no risk of damaging a bone graft or endoprosthesis, which are necessary parts of having limb-sparing surgery.
Disadvantages of amputation include:
having to use an artificial limb
- being upset about the appearance of the stump
- phantom pain
Phantom pain is when you can still feel pain or other sensations in the limb that was removed. It occurs when nerves are cut and damaged during surgery, which causes the body to send abnormal nerve impulses. Symptoms of phantom limb pain include pain, burning, throbbing or itching. Symptoms are usually worse when there was a lot of pain in the limb before the amputation. Sometimes medicines can help to ease the sensation, and symptoms usually improve when a prosthesis is worn regularly.
In some cases, the child can be provided with something called an immediate fit prosthesis while still under anesthesia. For example, in the case of a leg amputation, a cast is put on what remains of the limb (the stump) in the operating room. A basic post with a foot is then attached. When waking from anesthesia, the child can look down and see 2 feet pushing up the covers. One to 2 days after surgery, the child can get up and start walking with crutches. This gives a big boost to their morale. The cast helps to control swelling of the stump and allows it to shrink to be ready for the permanent prosthesis in a shorter time frame. It takes about 3 to 4 weeks after surgery for the swelling to decrease enough for the first fitting for a permanent prosthesis.
Specialized joints and devices that help a permanent prosthesis function as naturally as possible are usually discussed later when the child is fully rehabilitated. These options allow children who have an amputation to remain physically active, participate in different sports and have a good quality of life.
Physiotherapy to learn to walk usually starts a few weeks after amputation. This timing, and how intense the physiotherapy is at first, depends on whether other treatments need to follow surgery. Exercises usually focus on getting the other limb as strong as possible, strengthening any part of the limb that remains and preventing the muscles or joints that remain in the amputated limb from shortening. It usually takes about 6 months for children to walk well after surgery. Active teens need a new artificial leg or prosthesis about every 2 years.
Limb-sparing surgery
Limb-sparing surgery removes a bone tumour in the arm or leg along with a wide margin of normal bone and tissue around the tumour without removing (amputating) the entire limb. Any tissue from or near the biopsy site is also removed along with the tumour. Limb-sparing surgery is also called limb-salvage surgery.
Limb-sparing surgery is not an option for all children who have a tumour in the arm or leg. This surgery may be possible if:
- The tumour responded to, or was smaller after, chemotherapy.
- There is enough skin and soft tissue to cover the wound after the tumour is removed. This often depends on where the biopsy was taken and whether or not it was planned along with surgery.
- The cancer has not spread to any major arteries, veins or nerves.
- The cancer hasn't weakened the bone and caused breaks (called pathological fractures).
The surgeon may need to take skin or tissue from another part of the body to replace the tissue that was removed along with the tumour. Using skin or tissue from another part of the body in this way is called a graft. This is often done at the same time as the limb-sparing surgery.
Reconstruction techniques for limb-sparing surgery
Surgeons will reconstruct the limb with a variety of techniques using bone, other tissues and metal implants. Reconstruction is done at the same time as surgery to remove the cancer. It is very common for a major surgery like this to lead to complications that then require more surgeries.
Surgeons may use some of the following materials for reconstruction:
A bone graft is a piece of bone taken from another part of the body. Metal rods, screws or plates may be used to secure the bone graft to the bone at the surgery site. Depending on the amount of bone needed, it may be taken from the child's own body (called an autograft) or from a donor (called an allograft). When an allograft is used, there is a higher chance that the bone won't heal properly (called non-union) and a higher chance of infection. Non-union of the bone can lead to fractures, and the child may need more surgery to fix the bone graft.
An endoprosthesis is an internal prosthesis or prosthetic implant placed in the remaining bone. An endoprosthesis is usually made of metal and plastic. It is used to replace joints that are removed by surgery, including the knee, shoulder and hip joints. Endoprostheses come in different types and sizes. Some can be expanded. A child who has an endoprosthesis may need surgery every 6 to 12 months to lengthen the endoprosthesis until the skeleton is fully grown.
Fusing the joint may be used for tumours in or near the knee or shoulder joint. This involves removing the joint surfaces and making the bones surrounding the joint one solid piece. The surgeon removes the whole joint and inserts a metal implant, such as a rod or plate, into the 2 remaining bone ends, joining the bone ends on each side of the removed joint. After a fusion, the joint no longer moves and the affected limb has to make up for the loss of motion.
Healing and rehabilitation after limb-sparing surgery
Having a bone graft or endoprosthesis means wearing a brace or cast after surgery for a lengthy period of time. The brace or cast supports the limb and limits how much it can be used. This allows time for healing and for the bone graft or endoprosthesis to join to the remaining bone in the limb.
Children who have limb-sparing surgery will need intensive rehabilitation and will take part in a rehabilitation program to be able to use the limb. It can take up to a year to learn to walk again after limb-sparing surgery in a leg.
Children may not be able to participate in some activities because bones with a bone graft or endoprosthesis may not be as strong as normal bones and joints. They may need more surgery later in life if the bone graft or endoprosthesis wears out or is damaged.
Rotationplasty
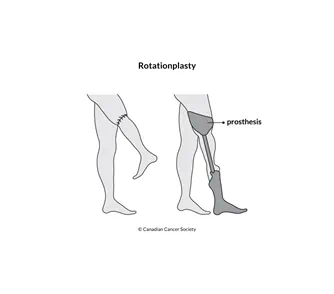
A rotationplasty may be used when the bone tumour is near the knee. In this procedure, the bone tumour is first removed from the lower thigh or upper leg by a wide resection. The surgeon then rotates the remaining limb 180 degrees so that the foot faces backward and re-attaches the parts together with a plate and screw or a rod. A prosthesis (artificial leg) can later be attached to the reconstructed limb, with the rotated ankle joint functioning as a new knee joint.
The only requirement for rotationplasty is that the sciatic nerve, which is the main nerve of the lower limb, cannot be near the tumour. If the main artery and vein are covered by the tumour, they can be cut and removed with the tumour. Following rotation, the main artery and vein will be reattached. When the child wakes up in the recovery room, they can usually wiggle their ankle and toes.
When the tissues have healed, usually after a month or so, a prosthesis is made for the child. The child's foot fits into a socket inside the prosthesis. When the foot pushes straight down, it moves the prosthesis up because the rotated ankle with the toes facing backward acts like a knee joint. When the foot and ankle lift up, it moves the prosthesis down.
Children with very large tumours involving large amounts of soft tissue around the bone often require an amputation above the knee to completely remove the tumour. A rotationplasty is a good alternative to an above-knee amputation as it gives the same function as an amputation below the knee.
Advantages of rotationplasty include:
- It uses a natural joint in the body and avoids the need for a mechanical knee joint, which does not work as smoothly. A mechanical knee joint is also more prone to breakage, particularly in a young, active child.
- There are no restrictions to high-impact activities and sports.
- The change in limb lengths as the child grows can be accommodated by adjusting the prosthesis length. For a very young child, this means a lot less surgery over time.
- A rotationplasty is very durable. There is nothing to wear out and future surgery is not necessary.
Many studies on quality of life have shown that children with rotationplasties are very satisfied.
Surgery for metastases
Sometimes surgery is done to remove bone cancer that has spread (metastasized) to the lung. Whether or not surgery is an option and the type of surgery done depends on:
the number of tumours (metastases)
- the size of the metastases and where they are in the body
- if the metastases are close to important blood vessels or the spinal cord
- the child's overall health
- whether or not the child is currently having chemotherapy
If surgery is an option for lung metastases, doctors often use a wedge resection to remove the metastasis along with a triangle-shaped piece of the lung around the tumour. Lobar resection or pneumonectomy are other options. Lobar resection removes the lobe of the lung that has the metastasis. Pneumonectomy removes all of the lung.
Side effects
Side effects can happen with any type of treatment for childhood bone cancer, but everyone's experience is different. Some children have many side effects. Other children have only a few side effects.
Side effects can develop any time during, immediately after or a few days or weeks after surgery. Most side effects will go away on their own or can be treated, but some may last a long time or become permanent.
Side effects of surgery will depend mainly on the type of surgery, the size and location of the tumour, how much tissue is removed, the child's age, as well as the child's overall health. Side effects also depend on the effects of other treatments. For example, tissue treated with radiation may not heal well after surgery. General side effects of surgery for bone cancer include:
- pain
- wound infection
- bleeding
- wound separation (edges of the wound don't meet together)
- nerve damage
- swelling in the limbs
- scarring
- phantom pain (if the limb has been amputated)
- non-union of the bone
Sometimes side effects develop months or years after surgery. Find out more about late effects of treatments for childhood bone cancer.
Tell the healthcare team if your child has any side effects you think might be from surgery. The sooner they are aware of any problems, the sooner they can suggest ways to help your child deal with them.
Questions to ask about surgery
Find out more about surgery and side effects of surgery. To make the decisions that are right for your child, ask the healthcare team questions about surgery.
