What is ovarian cancer?
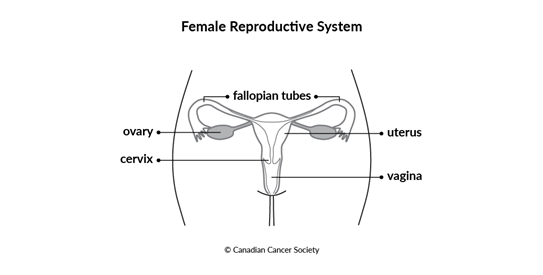
The ovaries and fallopian tubes are part of the female reproductive system. The ovaries produce eggs and make sex hormones in pre-menopausal women. During the menstrual cycle, an egg travels through a fallopian tube from the ovary to the inside of the uterus.
There are 2 ovaries. Each one is located deep in the pelvis on either side of the uterus (womb), close to a fallopian tube. There are 2 fallopian tubes on either side of the uterus.
Cells in an ovary or fallopian tube sometimes change and no longer grow or behave normally. Changes to ovarian cells may lead to non-cancerous (benign) conditions such as cysts. They can also lead to non-cancerous tumours, such as benign epithelial ovarian tumours.
Changes to cells in a fallopian tube can cause a precancerous lesion called serous tubal intraepithelial carcinoma (STIC). Precancerous means that the abnormal cells are not yet cancer, but there is a chance that they will become cancer if they aren't treated.
In some cases, changes to cells of an ovary or fallopian tube can cause cancer. A
cancerous (malignant) tumour is a group of cancer cells that can grow into nearby
tissue and destroy it. The cancer cells can also spread (metastasize) to other parts
of the body. Most ovarian cancers start in the epithelial cells. These cells are
found in the tissue that covers each ovary and lines the fallopian tubes and
It's often hard to know if cancer started in the ovaries. Most epithelial ovarian cancers are now thought to start in the nearby fallopian tube, but it’s very difficult to find cancer there.
Fallopian tube cancer and primary peritoneal cancer are very similar to epithelial ovarian cancer. They start in epithelial tissue, cause the same symptoms, and are staged and treated the same way. But they are much less common than ovarian cancer.
Other than epithelial ovarian cancer, rare types of ovarian cancer can also develop. These include germ cell ovarian cancer and stromal cell ovarian cancer.
The ovaries and fallopian tubes
The ovaries are the organs in a woman’s reproductive system that produce eggs (ova). There are 2 of them, and they are deep in a woman’s pelvis, on both sides of the uterus (womb), close to the ends of the fallopian tubes.
Structure
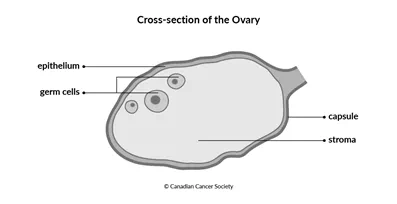
Different types of cells and tissue are found in the ovaries.
The epithelium
is the tissue that covers the ovary. It also lines the fallopian tubes and
Germ cells are inside the ovary. They develop into eggs.
The stroma is the supportive or connective tissue of the ovary. It is made up of stromal cells.
The capsule is a thin layer of tissue that surrounds each ovary.
What the ovaries and fallopian tubes do
The ovaries have 2 main functions. They make the sex hormones estrogen and progesterone. They also produce eggs.
During ovulation each month, an ovary releases an egg. The fallopian tubes carry the egg from the ovary to the inside of the uterus. If the egg is fertilized by a sperm, the egg attaches itself to the lining of the uterus (called implantation) and begins to develop into a fetus. If the egg is not fertilized, it's shed from the body along with the lining of the uterus during menstruation.
During menopause, the ovaries stop making sex hormones and releasing eggs.
Cancerous tumours of the ovary
Serous tubal intraepithelial carcinoma (STIC)
Borderline ovarian tumours
Non-cancerous tumours and conditions of the ovary
Your trusted source for accurate cancer information
With support from readers like you, we can continue to provide the highest quality cancer information for over 100 types of cancer.
We’re here to ensure easy access to accurate cancer information for you and the millions of people who visit this website every year. But we can’t do it alone.
Every donation helps fund reliable cancer information, compassionate support services and the most promising research. Please give today because every contribution counts. Thank you.
