Chemotherapy for brain and spinal cord tumours
Chemotherapy uses anticancer (cytotoxic) drugs to destroy cancer cells. It is sometimes used to treat brain and spinal cord tumours. Your healthcare team will consider your personal needs to plan the drugs, doses and schedules of chemotherapy. You may also receive other treatments.
Chemotherapy is given for different reasons. You may have chemotherapy to:
- destroy cancer cells left behind after surgery and reduce the risk that the cancer will come back (recur) (called adjuvant chemotherapy)
- treat recurrent tumours after or along with radiation therapy
- treat cancer that has spread to the spine from other areas of the body
Chemotherapy is usually a systemic therapy. This means that the drugs travel through the bloodstream to reach and destroy cancer cells all over the body, including those that may have broken away from the primary tumour in the brain or spinal cord. Brain tumours are different from most other types of cancer because they rarely spread outside the central nervous system (CNS) to other parts of the body. They may spread to nearby tissue in the area where they begin.
The blood-brain barrier is a protective network of blood vessels and cells that filters blood flowing to the brain. This barrier makes it hard for some substances (such as anticancer drugs) to enter the brain. It prevents many chemotherapy drugs from reaching brain tumour cells in large enough amounts to destroy them. The chemotherapy drugs used to treat brain tumours must be able to cross the blood-brain barrier.
Regional chemotherapy
Chemotherapy may also be a regional therapy, which means that it is given to a specific area of the body.
Intraventrical chemotherapy
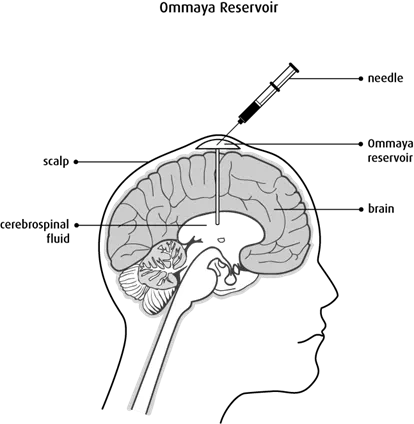
Chemotherapy for brain tumours may be given directly into the cerebrospinal fluid (CSF) in the ventricles of the brain. It is given through an Ommaya reservoir, which is a small, dome-shaped device with a short tube (catheter) attached to it that is placed during surgery. The chemotherapy drug is injected using a small needle inserted through the scalp into the Ommaya reservoir.
Intrathecal chemotherapy
Chemotherapy may be given through a lumbar puncture into the space around the spinal cord containing CSF.
Localized chemotherapy
With some types of brain tumours, the surgeon may line the area where the tumour was removed with special wafers (glial wafers or Gliadel). These wafers have concentrated doses of the drug carmustine (BiCNU, BCNU), which is released into the brain tissue as the wafers break down.
This method of chemotherapy delivers a concentrated amount of the chemotherapy drug to the area where the tumour was in the brain, while limiting the amount of normal cells in the body affected by the drug.
Chemotherapy drugs used for brain and spinal cord tumours
The most common chemotherapy drugs used to treat brain and spinal cord tumours are:
- temozolomide (Temodal)
- carmustine
- lomustine (CeeNU, CCNU)
- cisplatin (Platinol AQ)
- carboplatin (Paraplatin, Paraplatin AQ)
- etoposide (Vepesid, VP-16)
- irinotecan (Camptosar)
- methotrexate
- procarbazine (Matulane)
- vincristine (Oncovin)
- cyclophosphamide (Cytoxan, Procytox)
The most common chemotherapy drug combination used to treat brain and spinal cord tumours is PCV (procarbazine, lomustine and vincristine).
Side effects
Side effects can happen with any type of treatment for brain and spinal cord tumours, but everyone’s experience is different. Some people have many side effects. Other people have few or none at all.
Chemotherapy may cause side effects because it can damage healthy cells as it kills cancer cells. If you develop side effects, they can happen any time during, immediately after or a few days or weeks after chemotherapy. Sometimes late side effects develop months or years after chemotherapy. Most side effects go away on their own or can be treated, but some side effects may last a long time or become permanent.
Side effects of chemotherapy will depend mainly on the type of drug, the dose, how it’s given and your overall health. Some common side effects of chemotherapy drugs used for brain and spinal cord tumors are:
- fatigue
- low blood cell counts (called bone marrow suppression)
- loss of appetite
- nausea and vomiting
- sore mouth and throat
- diarrhea
- constipation
- hair loss
- skin problems
Tell your healthcare team if you have these side effects or others you think might be from chemotherapy. The sooner you tell them of any problems, the sooner they can suggest ways to help you deal with them.
Information about specific cancer drugs
Details on specific drugs change regularly. Find out more about sources of drug information and where to get details on specific drugs.
Questions to ask about chemotherapy
Find out more about chemotherapy and side effects of chemotherapy. To make the decisions that are right for you, ask your healthcare team questions about chemotherapy.
